How Hysteroscopy Surgery Can Help Diagnose and Treat Uterine Issues
Women, many times, ignore when something doesn’t feel right in the area around their uterus. For many women, experiencing unusual bleeding, fertility challenges, or unexplained pelvic pain can go unnoticed with the source of the problem hidden from view. Hysteroscopy, a medical procedure that allows doctors to see directly inside the uterus without major surgery, changes this scenario. This minimally invasive technique not only helps to diagnose conditions like fibroids, polyps, and endometrial thickening but can often treat them during the same procedure. This gives women clarity, information, and solutions to empower them to take charge of their reproductive health in a more meaningful way. Here is everything you need to know about hysteroscopy:
Introduction to Hysteroscopy Surgery
What is a hysteroscopy?
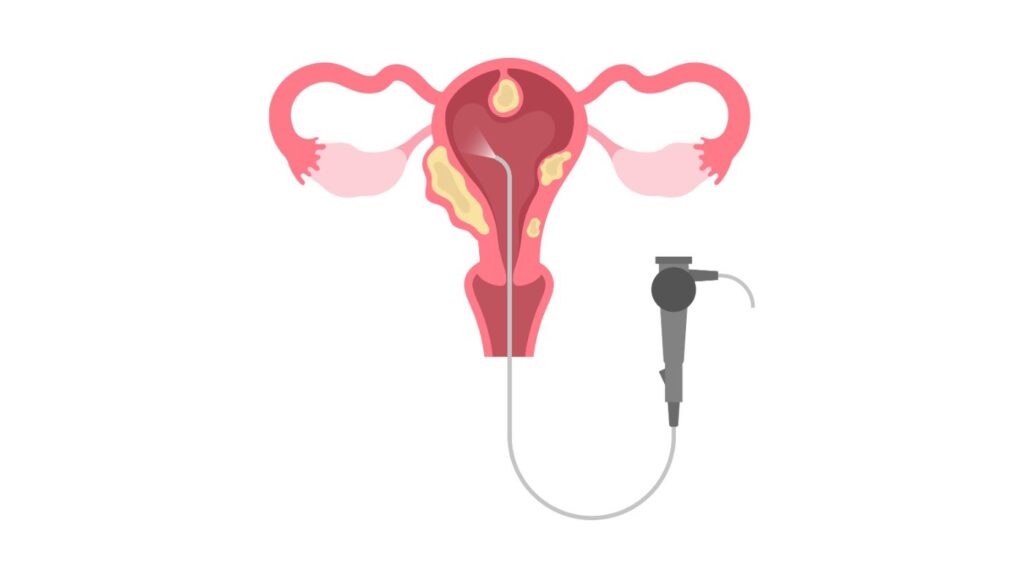
A hysteroscopy procedure is a minimally invasive technique that doctors use to diagnose and treat various uterine and cervical conditions, like abnormal uterine bleeding, abnormal endometrial thickening, postmenopausal bleeding and infertility. The hysteroscopy procedure allows the doctor to look inside the uterus with a hysteroscope, which is a thin, lighted tube that is inserted through your vagina to examine the cervix and the inside of the uterus. Hysteroscopy can be used for diagnosis or treatment.
The role of hysteroscopy in diagnosing uterine issues
Hysteroscopy that is part of the diagnostic process is known as diagnostic hysteroscopy. Diagnostic hysteroscopy plays a very important role in diagnosing uterine issues as it gives visual access of the uterine cavity and allows doctors to identify and assess any abnormalities like fibroids, polyps, adhesions and any other structural irregularities that can cause symptoms like abnormal uterine bleeding, or infertility related issues.
Types of Hysteroscopy
Diagnostic hysteroscopy vs. operative hysteroscopy
Diagnostic hysteroscopy is used to examine the insider of the uterus and cervix to diagnose potential issues affecting reproductive health. A hysteroscopy procedure, in this case, can be used to confirm other test results like an ultrasound. If necessary, a biopsy can be taken during the procedure for further examinations. If an issue is detected, then operative hysteroscopy may be performed simultaneously to treat the condition.
Therefore, a diagnostic hysteroscopy is for viewing only and an operative hysteroscopy is for both viewing and treating issues found within the uterus. While a diagnostic hysteroscopy is used to identify and confirm the cause of any uterine concerns, operative hysteroscopy is used to correct those abnormalities that were detected during the previous diagnostic hysteroscopy procedure.
Diagnostic hysteroscopy involves the use of hysteroscope but an operative hysteroscopy involves additional instruments like scissors, graspers, or electrocautery tools to remove tissue.
When is a diagnostic hysteroscopy performed?
Doctors use diagnostic hysteroscopy to investigate symptoms like heavy or irregular periods and unusual vaginal bleeding, as well as diagnose conditions including
- Abnormal endometrial thickening
- Postmenopausal bleeding
- Blocked fallopian tubes
- Endometrial cancer
- Intrauterine adhesions (IUAs), or scar tissue in the uterus
- Infertility
The Hysteroscopy Procedure
Step-by-step explanation of the procedure
A hysteroscopy procedure is typically performed as an outpatient procedure during a short hospital stay, depending on your condition and your healthcare provider’s approach. It is a minimally invasive procedure which involves inserting a hysteroscope into the uterus for diagnosis or treatment. Here is a step-by-step guide for the procedure”
- As is important with any procedure, the patient needs to be positioned properly to ensure there is no nerve injury. The patient has to lie on their back with the legs spread apart and bent at the knees for the hysteroscopy procedure to begin.
- The vaginal area will be cleaned with an antiseptic solution to prevent any infection.
- In some cases, the doctor may dilate or widen the cervix to make it easier to insert the hysteroscope.
- The doctor will gently insert the hysteroscope into the vagina, passing through the cervix into the uterus.
- A liquid (saline) or gas (carbon dioxide) is injected through the hysteroscope to expand the uterus and improve visibility.
- The doctor will then look for any abnormalities like fibroids, polyps, or any other abnormal tissue growth.
- Biopsy samples will be collected, if required, for further testing.
- If it is an operative hysteroscopy, the doctor will further insert specialised tools to remove fibroids, polyps or adhesions.
- Once the examination is done, the doctor will remove the hysteroscope.
Preparation and anesthesia used during hysteroscopy
Preparation for a hysteroscopy depends on the type of hysteroscopy procedure and whether it’s done in an office or an operating room.
- You will need to fast for a few hours before the surgery and may be asked to empty your bladder.
- An IV line may be placed to administer fluids or any other medication.
- You may also need to avoid alcohol 24 hours before your hysteroscopy procedure.
- The doctor may ask you to not take any medication that increases the risk of bleeding.
- The procedure can be done with local anesthesia, sedation or general anesthesia, depending on the complexity of the procedure.
Normal vs. Abnormal Hysteroscopy Findings
What is considered a normal hysteroscopy result?
Normal hysteroscopy results would include a non-vascular smooth level and no structural irregularities. Abnormal findings may include polyps, submucosal myomas, fibroids, scar tissue, endometrial hyperplasia, and endometrial cancer.
Common uterine issues detected through hysteroscopy
- Fibroids: Non-cancerous growths in the uterine wall that can cause heavy bleeding or discomfort
- Polyps: Small, abnormal growths in the lining of the uterus, which may lead to irregular bleeding
- Adhesions: Scar tissue inside the uterus that can cause infertility or recurrent miscarriages.
- Endometrial Hyperplasia: A precancerous condition that involves thickening of the uterine lining.
- Uterine Septum: A congenital abnormality where a fibrous or muscular wall divides the uterus, affecting pregnancy outcomes.
How Hysteroscopy Can Treat Uterine Problems
Surgical interventions during hysteroscopy
Any surgical intervention during a hysteroscopy procedure are minimally invasive, used to treat various uterine issues without the need for larger incisions. Specialised instruments are inserted through the hysteroscope to perform treatments directly within the uterus. Another intervention can be removing a small sample of tissue from the uterine lining to further diagnose endometrial hyperplasia.
Removal of fibroids, polyps, and adhesions
Some common surgical treatments performed during hysteroscopy include:
- Removal of Fibroids: Uterine fibroids can be removed or reduced surgical instruments which can alleviate symptoms like heavy bleeding.
- Removal of Polyps: Polyps can be excised during hysteroscopy, which can help with irregular bleeding or fertility issues.
- Removal of Adhesions: Adhesions can be broken up or removed to restore uterine structure and improve fertility.
What to Expect After a Hysteroscopy
Post-procedure care and recovery timeline
- If general anesthesia was used during the hysteroscopy procedure, then you should consider taking a few days off. In most cases, the recovery timeline is within 1-2 days.
- Some common post-procedure sensations are cramping (similar to period pain) and some spotting or bleeding for a few days. This is usually considered normal, unless the bleeding is heavy.
- Avoid any sexual activity, using tampons, or douching for at least two weeks after the procedure to reduce the risk of infection.
- Avoid hot tubs, baths and swimming during recovery.
Common sensations and discomfort after hysteroscopy
- Feeling bloated
- Light bleeding for a few days
- Spotting
- Mild cramping
- Vaginal discharge
Potential Side Effects of Hysteroscopy
Short-term side effects to be aware of
As mentioned above, you might experience mild cramping or spotting after the procedure. Some other side effects may be:
- Stomach pain
- Lightheadedness or dizziness
- Mild nausea
- Shoulder pain
How to manage pain and discomfort
Pain relief: Over-the-counter pain relievers like ibuprofen can manage mild cramping or discomfort.
Heat therapy: A heating pad on lower abdomen can also ease cramping
Rest: You must take rest for at least a day after the procedure and avoid any strenuous activities.
Hydration: Drink a lot of water to help ease any bloating or discomfort.
Signs of Infection After Hysteroscopy
Recognizing signs of infection and complications
While hysteroscopy is considered to be a safe procedure, it can also lead to complications like any other surgery. Some of the complications include
- Infection
- Heavy bleeding
- Intrauterine scarring
- Bad reaction to anesthesia
- Injury to the cervix, uterus, bowel or bladder
- Bad reaction to the saline or other substance used to expand the uterus
Infection is one of the major risks after a hysteroscopy and therefore its important to recognise its signs that include
- Severe abdominal pain
- High fever
- Foul-smelling discharge
- Dizziness or fainting
When to seek medical help
If you experience any of the above mentioned symptoms, you should immediately contact your service provider for further evaluation and treatment. Early intervention is essential to avoid any serious complications.
Benefits and Risks of Hysteroscopy Surgery
Advantages of hysteroscopy in uterine diagnosis and treatment
- A hysteroscopy surgery is less invasive than traditional surgery, meaning smaller incisions or no incisions at all, which leads to quicker recovery and minimal scarring.
- The procedure gives a clear view of the uterine cavity which allows the doctor to accurately diagnose conditions like endometrial hyperplasia, fibroids, polyps, and adhesions.
- Diagnostic and Hysteroscopy surgery can be performed simultaneously.
- Hysteroscopy can improve reproductive health and fertility in many cases.
Risks and potential complications
- Like discussed above, there is a risk of infection in the uterus cervix or vaginal area.
- The hysteroscopy may puncture the uterine wall leading to injury or bleeding
- Heavy bleeding in some cases requires additional medical attention
- An adverse reaction to anesthesia can be one of the complications especially if the patient is allergic.
- In rare cases, the procedure might cause new scar tissue which can affect fertility.
Conclusion
Hysteroscopy surgery is a valuable tool for diagnosing and treating uterine conditions, offering a less invasive approach to addressing issues like endometrial hyperplasia. It allows for accurate diagnosis and effective treatment, helping improve reproductive health outcomes. While the procedure is generally safe, patients should be aware of potential risks such as infection and heavy bleeding.
For expert guidance and personalized care, visit Ovum Fertility Hospital and consult a fertility specialist in Bangalore to explore the best treatment options for your reproductive health.
FAQ
1. Is hysteroscopy the same as D&C?
No, they are not the same. A hysteroscopy is a surgical procedure to remove fibroids or polyps from the cavity of the uterus, and dilation and curettage (D&C) is performed to remove tissue from the inner lining of the uterus.
2. Is a hysteroscopy procedure painful?
Most patients experience mild discomfort or cramping, but pain is generally manageable with over-the-counter medication.
3. Are there any risks with hysteroscopy surgery?
Risks include infection, heavy bleeding and anesthesia complications.
4. Can hysteroscopy treat infertility?
Yes, hysteroscopy can be performed to treat conditions like adhesions and fibroids that affect fertility.